CMS’ FY 2010 Report to Congress On the RAC Program
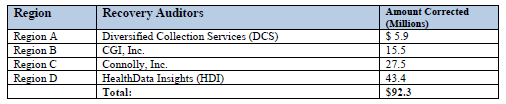
The Centers for Medicare and Medicaid Services (“CMS”), as required by Section 6411 of the Patient Protection and Affordable Care Act (“PPACA”), must annually report to Congress “concerning the effectiveness of the Recovery Audit Contractor program under Medicaid and Medicare and shall include such reports recommendations for expanding or improving the program.” In its FY 2010 Report to Congress Regarding the Recovery Audit Contractor (“RAC”) Program (“Report”), the Recovery Auditors identified and corrected combined overpayments and underpayments totaling $92.3 million–82% of which were overpayments and 18% of which were underpayments. CMS provided a breakdown of amounts corrected by region and Recovery Auditor:
Most notably in the Report are the audit statistics in which CMS stated, “[h]ealth care providers have appealed 8,449 claims to date, which constitutes 5 percent of all claims collected in FY 2010. Of those, 2,902 claims–2.4 percent of all collected claims–were ruled in the providers’ favor, for a total overturned amount of $2.6 million.” Based on these figures, over 34 percent of the appealed claims already have been ruled in the providers’ favor. It should also be noted that the appeals process can take up to two (2) years. The reported data represents appeals results to date of the claims originating and appealed in FY 2010.
CMS provides the following table elaborating on the FY 2010 RAC appeals statistics:
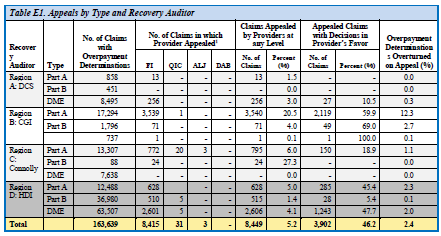
CMS also identifies “issue codes” or “major findings,” which are vulnerabilities tracked and identified through the RAC program. CMS states it posts its major findings to “allow providers to understand where improper payments are occurring so they can develop additional corrective actions.”
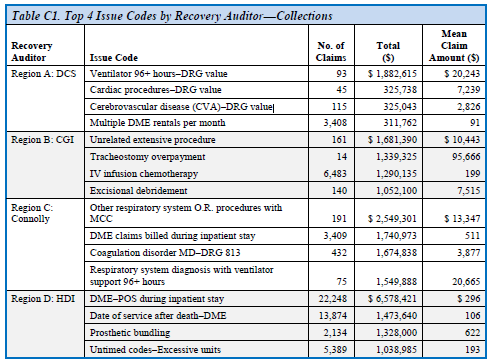
Finally, the Report also contains a number of other helpful appendices including tables breaking down improper payments by state; region/Recovery Auditor; and Medicare Part A, B, and DME claims.
For more information on RACs and audit appeals, please contact Abby Pendleton, Esq. or Jessica L. Gustafson, Esq. at (248) 996-8510 or (212) 734-0128 or visit the HLP website.
 Health Law Attorney Blog
Health Law Attorney Blog

